  
This rapid heart rate in the ventricles can then lead to similar symptoms of AFib with palpitations or shortness of breath. This still results in the heart beating between 120 and 170 times per minute. Many times only every other beat from the atria makes it through to the ventricles. Fortunately, they usually do not beat quite as fast as the atria. The lower chambers of the heart, the ventricles, also beat faster than normal. However, having atrial flutter in the right atrium is more typical form of atrial flutter. There are also less common forms of atrial flutter where the short circuit travels in the left atrium, not the right atrium. These rapid contractions can prevent the chambers from filling completely between heartbeats. In the most typical form of atrial flutter, a short circuit forms allowing the electrical signal to travel rapidly around the right atrium at a typical speed between 240 and 340 contractions per minute. The electrical impulse then travels through the heart muscle, triggering it to squeeze. The normal beats begin with an electrical signal sent out from a small area in your heart’s right upper chamber (atrium) called the sinus node. Normally your heart beats between 60 and 100 times per minute. While atrial flutter shares many similarities with AFib, there are a few key differences to discuss. There are so many similarities that I frequently refer to atrial flutter as the cousin of atrial fibrillation. Both arrhythmias can cause a rapid heart rate and increase risk for stroke. 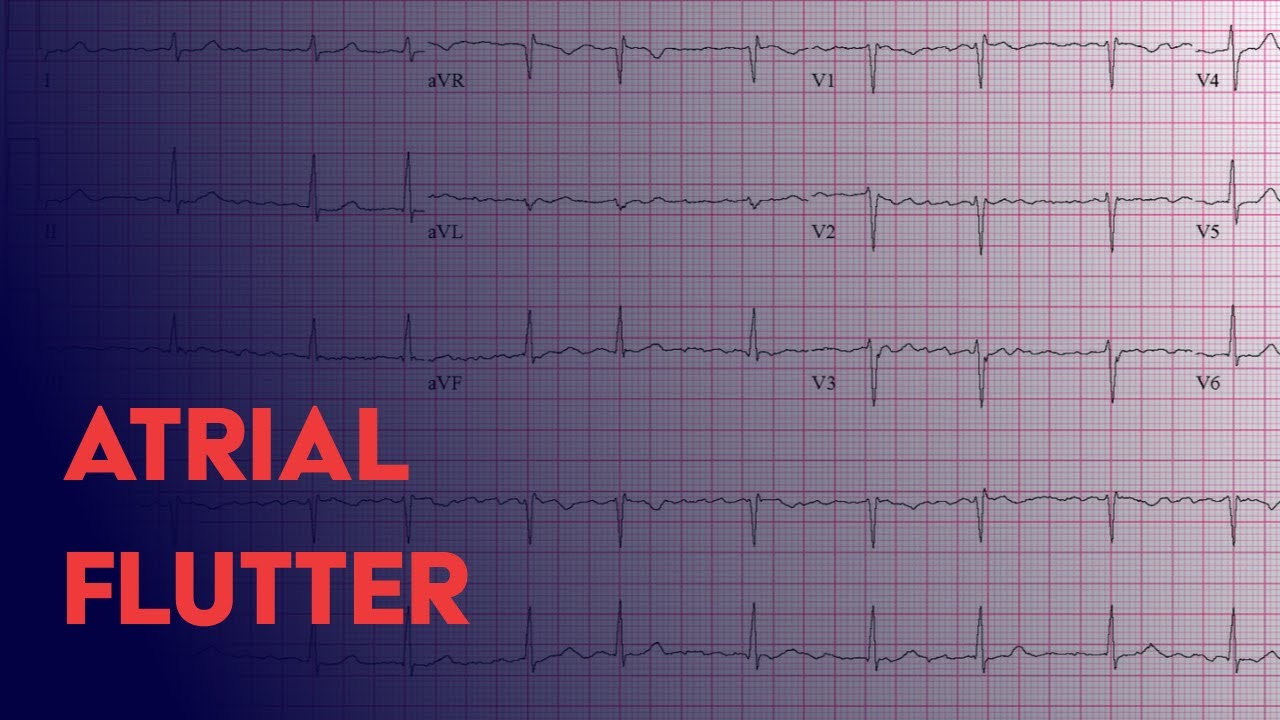
Another common heart arrhythmia is called atrial flutter. While atrial fibrillation ( Also known as AFib) is one of the better-known heart rhythm disorders, it isn’t the only one. It has been updated.ĭownload a copy of the guide: 10 tips to identify atrial flutter.What You Should Know About Atrial Flutter Read next: Training Day: Mastering the 12-lead With these tips and practice, you will be much less likely to mistake atrial flutter with 2:1 conduction for another tachycardia. You will learn to see the rhythm strip as separate atrial activity and ventricular activity portions and the hidden flutter waves will stand out for you. Look at as many strips of confirmed 2:1 conduction as you can and your eye will become trained to see it. Now that you are more aware of atrial flutter with 2:1 conduction, the best way to get good at recognizing it is regular practice. You might consider using a Lewis lead, which enhances detection of atrial activity. In some leads, atrial flutter will not have a sawtooth pattern. A 12-lead ECG can help immensely in seeing the flutter waves, because some leads are better for viewing atrial activity than others. 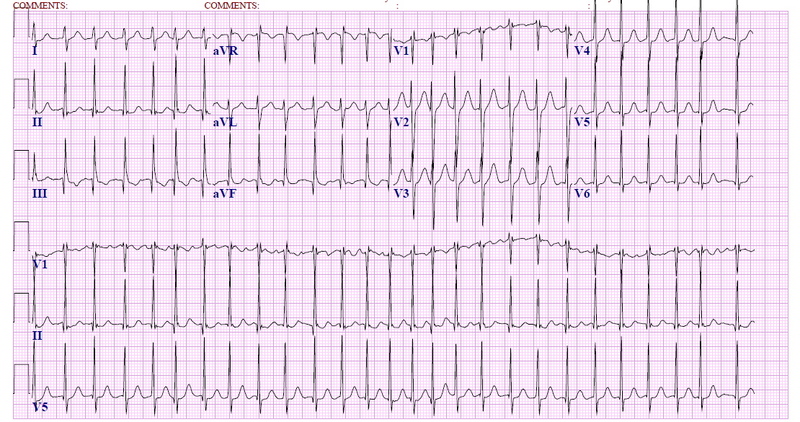
Use more than one leadįor rhythm interpretation, the more leads the better. By evaluating the P waves, QRS complexes, intervals and rate, you may discover that your first impression was wrong. Get your first impression, then think of alternate diagnoses and apply rhythm interpretation criteria. Most people with sinus tach, especially over 130 bpm, will usually have a readily-apparent reason for the tachycardia, like fever, fear, pain, anxiety, exertion, drugs, hypovolemia or hypoxia. You see no obvious reason for sinus tachycardiaĬonsider atrial flutter if the patient has no obvious reason for sinus tachycardia. Re-entrant tachycardias hit a fast rate suddenly and maintain that rate until they end suddenly. For example, if your patient talks or moves around in bed, the rate may go up slightly. Remember that sinus rhythms tend to fluctuate slightly. Suspect any tachycardiaĪny rhythm around 150 bpm should be suspected of being atrial flutter with 2:1 conduction. Here are 10 tips to avoid missing atrial flutter. You won't find atrial flutter it if you aren’t looking for it. 10 tips to avoid missing atrial flutter with 2:1 conduction. As cardiac output is decreased and cardiac workload increased, ventricular fibrillation can result. In patients with accessory pathways that bypass the slow conduction of the AV node, like Wolff-Parkinson-White Syndrome, 1:1 conduction of atrial flutter or atrial fib can be life-threatening. Atrial flutter can lead to fast rates at 2:1 conduction, and VERY fast rates at 1:1 conduction. When we see slower ventricular rates and conduction ratios of 3:1 or more, it is usually due to medications or other causes of enhanced refractoriness of the AV node. New-onset atrial flutter is most often conducted 2:1, because that is a comfortable rate (around 150 per minute) for the AV node to conduct. The AV node is bombarded by a regular atrial rhythm of around 300 per minute. It can occur suddenly, and is sometimes associated with periods of atrial fibrillation. Atrial flutter is a re-entrant tachycardia that occurs in the atria. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
